Case studies
Social Movement Action Framework
Strengthening health systems: The experience of the National Health Forum in El Salvador (2009 - 2018)
A nationwide social movement in El Salvador from 2009 to 2018 supported the achievement of the National Health Forum and exemplified goals and outcomes being met by activists. Read more in this case study.
The National Health Forum (NHF), a nationwide popular movement in El Salvador, played a central role in the development of the National Public Health System from 2009 to 2018 (León et al., 2020). It is part of a global movement that aims to build coalitions and networks. The People’s Health Movement (PHM) brought together grassroots health activists, civil society organizations and academic institutions from around the world to address the social, environmental, and economic determinants of health (Kapilashrami et al., 2016).
The NHF provides a strong example of community participation and exemplifies a social movement with fully achieved goals. Formally created in 2010, the NHF had three fundamental goals that were met via social movement actions:
- to build people’s power and strengthen the organizational fabric
- to stand against the idea that previous governments held of privatizing health care
- to stimulate and promote effective social participation in health
The NHF developed three community participation strategies that played a role in strengthening El Salvador’s national public health system. These strategies are: (1) building capacity among local community leaders to become effective decision-makers at all levels of the health-care system, (2) responding to and prioritizing the needs identified by the community for the sector-specific working groups, and (3) advocating for policies based on human rights.
“The NHF was born with high participation of different social movements, all united in the same direction. There were a series of problems, as they wanted to privatize health care […] The NHF was created when the health reform came into being. We, the NHF, are part of the reform” – NHF member

Advocating for change through the Alzheimer's Association
The Alzheimer's Association was started by activists committed to advancing Alzheimer's knowledge through research.
The Alzheimer’s Association (Alzheimer's Association | Alzheimer's Disease & Dementia Help) was founded in 1980 by a group of family care providers and individuals who supported the need for an organization dedicated to support the needs of caregivers facing Alzheimer’s and to advance knowledge through research. As early activists for the Alzheimer’s movement, they sought to break down the silence of Alzheimer’s and learn more about the disease, including prevention, treatment and a cure.
Through a people-led approach, the association reaches millions of people globally through a multi-pronged approach grounded in individual and collective action. Advocacy to give all persons living with Alzheimer’s access to the support services they need includes strategies such as launching awareness campaigns and grassroots campaigns to impact legislation.
With multiple chapters throughout North America and globally, the Alzheimer’s Association includes a network of advocates and allies. These include other Alzheimer’s organizations, universities engaged in research, corporations and pharmaceuticals. As an example of a civil society organization, the Alzheimer’s Association is a community-based non-profit organization that has protected and advocated for the needs and interests of persons and families living with Alzheimer’s for over 40 years.

Scaling up change to address hunger and food waste through The Campus Kitchens Project
The Campus Kitchens Project was an effective scaled up change initiative that addressed food insecurity. read more in this case study.
The Campus Kitchens Project (CKP) is an example of a successful scaled-up change initiative. Founded in 2001 as a branch of a community kitchen initiative that targeted food insecurity in Washington, D.C., United States, this non-profit is the first and largest student-led social movement taking on the crisis of food waste and hunger in the United States (Larson et al., 2017). More than 30,000 students in 63 universities, colleges and high schools are now repurposing unwanted or surplus food to provide meals to people who have food insecurity.
Working in leadership teams, student leaders and volunteers on campuses receive education, training and coaching over a period of several months to help empower people, families and communities on topics including:
- food insecurity
- improving social and nutritional health by increasing food knowledge and helping others developing cooking skills
The Campus Kitchen Project also establishes community partnerships with existing local organizations that provide services and food to individuals already challenged with food insecurity, such as senior housing facilities, youth outreach groups and churches. Local leadership teams also partner with dining services that operate large foodservice kitchens and dining halls and engage student groups and faculty advisors.
Student teams carry out different functions. While some teams focus on improving the way that homeless shelters prepare and deliver meals, other teams host communal dinners, partner with senior centers, or improve transportation to improve access to food.
“Instead of more branch offices or trying to provide all the services in-house, we find universities and students to partner with who already have the necessary resources on campus and want to do this kind of community impact work. Turning our nation’s institutions of higher education into hubs for replication and ongoing innovation could be the superhighway to scaling up for any nonprofit.” - Laura Toscano, Director, The Campus Kitchens Project

Knowledge-to-Action Framework
Applying the Knowledge-to-Action Framework to reduce wound infections at Perley Health
A case study on reducing wound infections at Perley Health in Ottawa, Ontario to advance best practices using the Knowledge-to-Action framework.
Perley Health is a designate Long-Term Care Best Practice Spotlight Organization® (BPSO®) which demonstrates a strong commitment to providing evidence-based care. During the pandemic, the team identified skin and wound infection as a clinical concern among their residents. Consistent with the literature, residents at Perley Health experiencing comorbid medical conditions such as frailty, diabetes, and arterial and venous insufficiency were at increased risk for chronic wound infections [1]. Chronic wounds are a prime environment for bacteria, including biofilm, making wound infection a common problem [2] [3]. Managing biofilm, which can affect wound healing by creating chronic inflammation or infection [3], becomes crucial as up to 80 per cent of infections are caused by this type of bacteria [4] [5].
To adopt and integrate best practices, the team at Perley Health decided to implement the Assessment and Management of Pressure Injuries for the Interprofessional Team best practice guideline (BPG). To support a systematic approach to change, four of the action cycle phases of the Knowledge-to-Action Framework, from the Leading Change Toolkit [6] are highlighted below.

Identify the problem
Perley Health’s wound care protocol was audited and the following gaps were identified based on current evidence:
- Aseptic wound cleansing technic could be improved, as nonsterile gauze was used for wound cleansing.
- Wound cleaning solution was not effective to manage microbial load in chronic wounds
- Baseline wound infection data were collected on the number of infected wounds within the organization each month over three years and is ongoing
Adapt to local context
The project was supported by key formal and informal leaders within the organization including the Nurse Specialized in Wounds, Ostomy and continence (NSWOC), the Director of Clinical Practice, a team of wound care champions, the IPAC team and material management. Staff was motivated to improve resident outcomes by lowering infection rates which facilitated the project but many continued to use old supplies so as to not waste material. Providing the rationale for the change and associated best practices improved knowledge uptake, as did removing old supplies to cut down on confusion. Barriers the team encountered included staff turnover and educating new team members.
Select, tailor, implement interventions
The interventions listed below were selected, tailored and implemented based on the evidence that was adapted to the local context. They were purposely chosen to support the clinical teams’ needs on busy units and to creatively overcome staffing challenges. Interventions included:
- use of a wound cleanser containing an antimicrobial
- use of sterile equipment for wound care, including sterile gauze
- creation of a wound-cleansing protocol was created to reflect best practice
- updating and approval of a policy by the Risk Assessment and Prevention of Pressure Ulcers team in collaboration with the director of clinical practice
Perley Health also created and delivered education in two formats designed to be accessible to front-line staff:
- Just-in-Time education was provided on every unit, on every shift, to registered staff by the NSWOC on all shift sets, over a one-month period. Wound care champions were available on each shift to aid in learning and answer additional questions to support the team’s needs.
- A continuing education online learning module was created and uploaded onto Perley Health’s Surge learning platform. Training is included in new hire onboarding and mandatory for yearly education.
Image
An RPN demonstrating how to cleanse a wound using wound cleanser at Perley Health
Evaluate outcomes
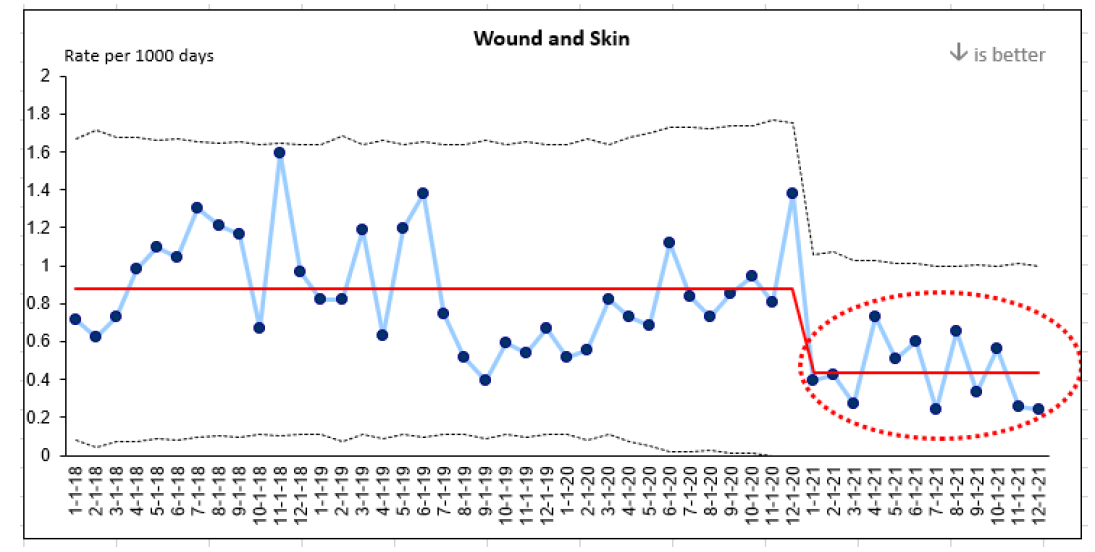
Evaluation indicators were selected to determine the impact of the implementation interventions when compared to baseline data, including the rate of wound and skin infections per 1,000 days. A 50 per cent reduction in wound infections was identified following the implementation of the identified change strategies and education above.
This graph represents four years of data collection on wound infections at Perley Health. Three years of baseline data and one year of post-implementation data are highlighted in red.
References
- Azevedo, M., Lisboa, C., & Rodrigues, A. (2020). Chronic wounds and novel therapeutic approaches. British Journal of Community Nursing, 25 (12), S26-s32.
- Landis, S.J. (2008). Chronic Wound Infection and Antimicrobial Use. Advances in Skin & Wound Care, 21 (11), p 531-540.
- Registered Nurses’ Association of Ontario (2016). Clinical best practice guidelines: Assessment and management of pressure injuries for the interprofessional team (3rd ed.). Registered Nurses’ Association of Ontario: Toronto, ON.
- Jamal, M., Ahmad, W., Andleeb, S., Jalil, F., Imran, M., Nawaz. M., Hussain, T., Ali, M., Rafiq, M., & Kamil, M.A. (2018). Bacterial biofilm and associated infections. J Chin Med Assoc. 81(1): 7-11.
- Murphy, C., Atkin, L., Swanson, T., Tachi, M., Tan, Y.K., De Ceniga, M.V., Weir, D., Wolcott, R., Ĉernohorská, J., Ciprandi, G., Dissemond, J., James, G.A., Hurlow, J., Lázaro MartÍnez, J.L., Mrozikiewicz-Rakowska, B., & Wilson, P. (2020). Defying hard-to-heal wounds with an early antibiofilm intervention strategy: wound hygiene. J Wound Care, (Sup3b):S1-S26.
- Registered Nurses’ Association of Ontario (2022). Leading change toolkit: Knowledge-to-action framework. https://rnao.ca/leading-change-toolkit Registered Nurses’ Association of Ontario: Toronto, ON.

Evaluating the impact of implementing the Person- and Family-Centred Care Best Practice Guideline at Spectrum Health Care
Spectrum Health Care, a Best Practice Spotlight Organization® (BPSO®) and home health organization, evaluated care outcomes after implementing the Person- and Family-Centred best practice guideline (BPG).
Spectrum Health Care (Spectrum), an RNAO Best Practice Spotlight Organization® (BPSO®), is a home health organization with more than 200 nursing staff across three locations in the province of Ontario, Canada.
Spectrum chose to implement the 2015 Person- and Family-Centred Care (PFCC) Best Practice Guideline (BPG) to enhance person- and family-centred care and to reduce complaints regarding care. Members of the senior leadership team at Spectrum Health Care led implementation together with Spectrum’s Patient and Family Advisory Council.
To support the practice change, Spectrum used the following implementation interventions:
- Conducting a gap analysis to determine the knowledge/practice gap;
- Holding education sessions for staff on person- and family-centred care best practices;
- Revising their care processes to include review of care plans with the person and/or members of their family
- Surveying staff members on their attitudes about person- and family-centred care via surveys
- Developing staff education on communication strategies to support the assessment of a person’s care needs and care plans.
After implementing these interventions, Spectrum assessed the number of complaints received from persons receiving care per 1,000 care visits and compared that to their baseline.
They found a decrease of 42 per cent of complaints from persons received over an 18-month time period at one of the sites that was implementing the PFCC BPG at Spectrum Health Care.
At another site, an 80 per cent reduction in complaints was found following the staff education intervention.
Data analyses overall indicated that the implementation of the PFCC BPG was highly successful in reducing persons' complaints regarding care.
Read more about Spectrum Health care’s results of implementing the PFCC BPG here: Slide 2 (rnao.ca)

Sustaining the Assessment and Management of Pain Best Practice Guideline across a multi-site long-term care home
The Region of Peel, a Best Practice Spotlight Organization® (BPSO®), has sustained the implementation of the Assessment and Management of Pain best practice guideline (BPG) for almost a decade.
The Region of Peel, an RNAO Best Practice Spotlight Organization® (BPSO®) started implementing the RNAO Assessment and Management of Pain best practice guideline (BPG) in 2014 and has sustained its use since then. For example, in their 2019 BPSO annual report, they cited a continuous downward trend in the number of clients who reported a worsening of their pain. Pain experienced by the residents was better controlled, and the staff was found to assess, identify, and manage pain better by using the BPG.
Their keys to success include:
- building on what works (for example, existing practices and policies)
- empowering champions and growing their champion network
- involving residents and families
- gaining support from leaders and partners including RNAO, Peel of Region Leadership, Health Quality Ontario).
- collaborating with an interdisciplinary team
- conducting a formal sustainability evaluation
To learn more about The Region of Peel’s journey in sustaining the use of the Assessing and Managing Pain BPG, along with other BPGs, check out this webinar.

